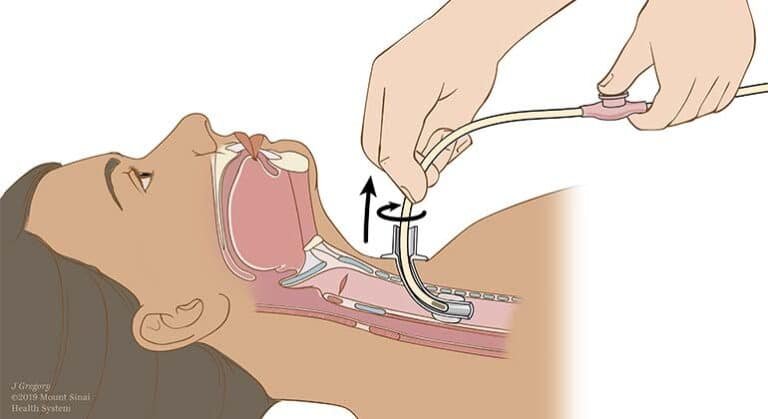
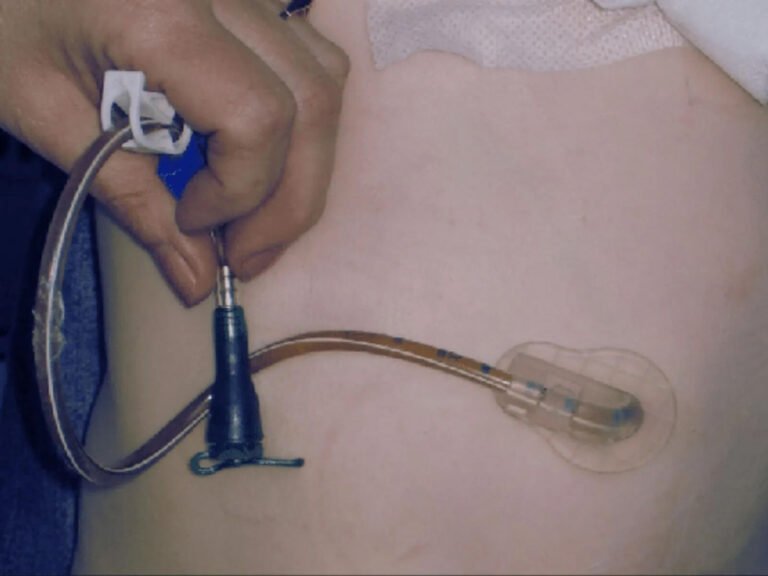
To prevent feeding tube clogs, you’ll need to flush your tube with 30 mL of water before and after each medication and formula administration. Flush every 4-6 hours during continuous feedings, and always use room-temperature water. Crush medications finely and dissolve them completely in warm water before administering. Prepare formula according to guidelines, shaking containers vigorously for two minutes. Choose larger-diameter tubes when possible, as they’re less prone to blockages. Understanding proper technique and emergency declotting methods will help you maintain ideal tube function.
Key Takeaways
- Flush tubes with 30 mL water before and after medications, every 4-6 hours during continuous feeds, and immediately after intermittent feedings.
- Crush tablets finely and dissolve in 15-30 mL warm water; flush with 30 mL water between each medication dose.
- Use room-temperature formulas, shake containers vigorously for two minutes, and inspect for separation or clumping before administration.
- Choose larger diameter tubes (10 French or larger) made of polyurethane or silicone to reduce clog risk.
- Document all flushes and interventions, monitor for early clogging signs, and collaborate with dietitians and nurses for optimal protocols.
Understanding Why Feeding Tubes Become Clogged
Feeding tube clogs develop through three primary mechanisms: medication residue buildup, formula precipitation, and inadequate flushing protocols. You’ll find that certain medications, particularly crushed tablets and thick suspensions, adhere to feeding tube materials and create obstructions.
When you mix incompatible formulas or medications, chemical reactions cause precipitation within the tubing. Understanding these clogging factors enables you to implement preventive strategies effectively.
Temperature changes also contribute to blockages, as cold formulas can solidify within tubes. Additionally, protein-based formulas tend to coagulate when exposed to acidic medications or gastric contents.
You must recognize that smaller-diameter tubes face higher clog risks due to reduced internal space. By identifying these underlying causes, you’ll better serve your patients through proactive tube maintenance and proper administration techniques.
Establishing a Consistent Flushing Schedule
To maintain tube patency, you’ll need to flush feeding tubes with 30 mL of water before and after each medication administration, every 4-6 hours during continuous feedings, and before and after formula delivery.
This flushing frequency prevents residue buildup that leads to occlusions.
Optimal timing matters greatly. Schedule flushes during natural care changes—shift changes, medication rounds, or feeding intervals.
Strategic flush scheduling during routine care transitions maximizes efficiency while maintaining consistent tube patency and preventing nutrition delivery interruptions.
Document each flush to guarantee accountability and identify patterns if clogs develop.
For patients receiving intermittent feedings, flush immediately after completion while residue remains fluid.
Don’t delay, as formula crystallizes quickly within tubes. Night flushes are equally critical; set reminders to prevent extended periods without irrigation.
Create individualized protocols based on formula viscosity, medication schedules, and tube type.
Consistency protects tube function and guarantees uninterrupted nutrition delivery for those you serve.
Proper Formula Preparation and Handling Techniques
When preparing formula, you’ll greatly reduce clog risk by following strict mixing protocols and maintaining proper temperatures.
Always use room-temperature water when reconstituting powdered formula, as cold water doesn’t dissolve particles completely. Shake containers vigorously for at least two minutes to guarantee thorough mixing without lumps.
Pay careful attention to formula storage guidelines—refrigerate opened containers immediately and discard after 24 hours.
Never use formula past its formula expiration date, as degraded components increase viscosity and clog potential. When shifting from refrigerated formula, allow it to reach room temperature naturally rather than using microwaves, which create hot spots that denature proteins.
Before administration, inspect your prepared formula for separation, clumping, or unusual consistency.
These signs indicate improper mixing or contamination that’ll compromise tube patency.
Safe Medication Administration Through Feeding Tubes
Medications pose one of the highest risks for tube occlusion, yet you can prevent most complications by crushing tablets properly and selecting appropriate formulations. Always verify whether medication types are suitable for tube administration before crushing or dissolving them.
| Medication Types | Preferred Dosage Forms | Administration Protocol |
|---|---|---|
| Tablets | Immediate-release, crushable | Crush finely, dissolve in 15-30mL warm water |
| Capsules | Powder-filled (opened) | Mix contents with water, flush thoroughly |
| Liquids | Sugar-free suspensions | Dilute thick preparations, avoid syrups |
Flush the tube with 30mL water before and after each medication. When administering multiple medications, flush between each dose to prevent interactions. Never mix medications together, as this greatly increases clogging risk and potentially reduces therapeutic effectiveness for your patients.
Choosing the Right Tube Size and Type
Larger feeding tubes resist clogging better than smaller ones, but selecting the ideal size requires balancing occlusion prevention with patient comfort and clinical appropriateness.
You’ll find that tubes 10 French or larger considerably reduce clog risk compared to smaller-bore options.
Consider tube materials carefully—polyurethane and silicone tubes offer superior flexibility and biocompatibility over PVC alternatives, minimizing irritation while maintaining patency.
Polyurethane and silicone tubes provide better flexibility and biocompatibility than PVC, reducing irritation while maintaining optimal patency.
These materials also resist medication adherence better than older formulations.
Evaluate tube lengths based on your patient’s anatomy and insertion site.
Longer tubes aren’t inherently problematic, but they require more diligent flushing protocols.
Document your rationale for tube selection, ensuring it aligns with the patient’s nutritional needs, expected duration of use, and individual tolerance.
Consult with your facility’s nutrition support team when uncertain about ideal specifications.
Water Quality and Temperature Considerations
Room-temperature water remains the gold standard for flushing feeding tubes, as it dissolves formula residue more effectively than cold water while avoiding the precipitation risks associated with hot water. You’ll need proper temperature control to maintain 68-77°F consistently. Consider water filtration systems if your patient has compromised immunity, as tap water may contain microorganisms that pose infection risks.
| Water Type | Temperature Range | Best Use Case |
|---|---|---|
| Filtered/Sterile | 68-77°F | Immunocompromised patients |
| Tap Water | 68-77°F | Standard patient care |
| Distilled | 68-77°F | High mineral content areas |
You’ll protect your patients by implementing these standards. Always verify water temperature before flushing, and document your filtration methods according to facility protocols. These simple measures greatly reduce clog formation while ensuring patient safety.
Recognizing Early Warning Signs of Tube Narrowing
Before complete obstruction occurs, you’ll notice subtle changes in tube performance that signal developing narrowing.
Watch for increased resistance when flushing—this requires more pressure than usual and indicates internal buildup. Formula delivery rates that progressively slow despite proper pump settings suggest partial blockage.
You’ll observe residue accumulation around connection sites and visible discoloration inside the tube during routine tube inspection.
Early symptoms include pump alarms triggering more frequently and formula backing up into extension sets.
Monitor feeding times carefully; sessions taking longer than baseline duration warrant immediate assessment. Your patients may report increased fullness or discomfort during feeds.
Document these changes systematically and implement aggressive flushing protocols before complete occlusion develops.
Regular tube inspection enables you to intervene early, maintaining nutrition delivery and preventing emergency replacements.
Emergency Declotting Methods When Prevention Fails
When a feeding tube becomes completely obstructed despite preventive measures, you’ll need to implement systematic declotting protocols immediately.
Start with warm water flushes using gentle pressure—never force the plunger, as this can rupture the tube. If ineffective, try pancreatic enzyme solutions mixed with sodium bicarbonate, allowing 30-60 minutes for enzymatic action.
Gentle warm water flushes come first—forcing pressure risks tube rupture. Pancreatic enzymes need 30-60 minutes to work effectively.
For medication-related clogs, carbonated beverages may help dissolve certain residues. These emergency techniques require careful documentation and physician notification.
If immediate solutions fail after repeated attempts, don’t delay replacing the tube—prolonged obstruction compromises nutritional delivery and increases aspiration risk.
Always maintain spare feeding tubes and declotting supplies in your care setting, ensuring you’re prepared to respond swiftly when prevention strategies fall short.
Special Considerations for Different Feeding Schedules
Your feeding schedule directly influences clog prevention strategies and requires tailored flushing protocols. Each regimen demands specific approaches to maintain tube patency and support ideal patient outcomes.
Continuous feedings require flushing every 4-6 hours during delivery and before/after medications. Nighttime feedings necessitate pre-sleep flushing and morning assessment to prevent formula stagnation during extended infusion periods.
| Schedule Type | Flush Frequency | Volume Per Flush |
|---|---|---|
| Continuous | Every 4-6 hours | 30 mL warm water |
| Bolus | Before/after each feeding | 30-60 mL warm water |
| Intermittent | Between feeding sessions | 30 mL warm water |
You’ll need to adjust protocols based on formula viscosity, tube diameter, and patient tolerance. Monitor residuals consistently, especially with nighttime feedings, to identify early clogging indicators and intervene promptly.
Working With Your Healthcare Team to Maintain Tube Patency
Maintaining tube patency requires consistent collaboration with multiple healthcare professionals who’ll monitor your tube function and adjust care protocols as needed.
Your dietitian will optimize formula selection and feeding schedules, while nurses provide hands-on guidance for flushing techniques and troubleshooting. Regular appointments with your physician guarantee early detection of mechanical issues before they escalate into complete blockages.
Effective team communication strengthens your ability to prevent clogs through coordinated interventions. Document any resistance during flushing, formula intolerance, or medication administration challenges, then share these observations promptly with your care team.
Track and report feeding resistance, formula reactions, and medication issues immediately to your care team for optimal tube maintenance.
This care coordination enables timely protocol adjustments based on your specific needs.
Don’t hesitate to request additional training sessions when you’re uncertain about proper maintenance procedures. Your proactive engagement directly impacts tube longevity and feeding success.
Conclusion
You’ve learned evidence-based strategies to keep your feeding tube functioning properly. By following consistent flushing protocols, preparing formula correctly, and administering medications safely, you’ll greatly reduce clog risks. Don’t hesitate to contact your healthcare team at the first sign of resistance—early intervention prevents complications. Remember, tube maintenance isn’t just about following rules; it’s about ensuring you receive uninterrupted nutrition. Stay proactive with your care routine, and you’ll maintain ideal tube patency.