When troubleshooting tube feeding complications, you’ll first assess for aspiration signs like coughing or respiratory distress, then verify tube placement using gastric aspirate pH and external markings. For blockages, flush gently with warm water using a 60mL syringe, progressing to enzyme solutions if needed. Address formula intolerance by reducing infusion rates and evaluating formula selection. Check equipment systematically for power connections, tubing alignment, and error codes. Proper documentation and systematic monitoring will guide your thorough approach to resolving these critical feeding challenges.
Key Takeaways
You’ve Got This: Help Is Just a Call Away
Taking care of someone with a feeding tube can feel overwhelming at times. You might worry when your loved one coughs during feeding, or feel frustrated when the tube gets blocked. These feelings are completely normal. You’re doing something important and challenging, and it’s okay to need support.
Think of tube feeding like learning to ride a bike. At first, everything seems complicated. But with practice and the right guidance, it becomes easier. Watch for signs that something might be wrong, like coughing or trouble breathing. Check how much food stays in the stomach to make sure your loved one is digesting well.
If the tube gets clogged, don’t panic. Try flushing it gently with warm water using a large syringe. Picture slowly melting away a blockage, the way warm water melts ice. Sometimes special solutions can help too.
When the formula causes upset stomach or discomfort, slow down the feeding. Imagine you’re being extra gentle, giving the body more time to adjust. Some people need easier-to-digest formulas, kind of like switching from a heavy meal to soup.
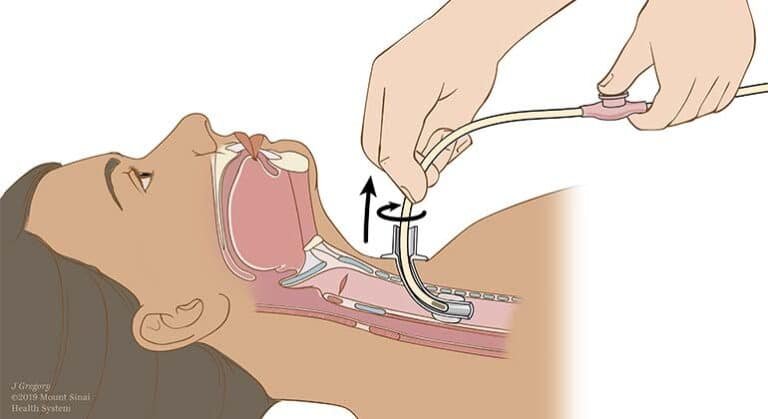
Always double-check that the tube is in the right place before feeding. It’s like making sure you’re on the right road before starting a journey. Test the liquid from the stomach and check the marks on the tube.
If the feeding pump shows an error, stay calm. Check all the connections like you’re solving a puzzle, one piece at a time. Keep backup supplies ready, just like keeping a spare tire in your car.
Remember, you don’t have to figure this out alone. Caring hands and expert knowledge are waiting to help you and your loved one feel safe and comfortable. If you or a loved one need help, don’t wait. Reach out to Skilled Trach Care today at (561) 677-8909 or email us at info@skilledtrachcare.com.
Identifying Common Tube Feeding Problems and Warning Signs
When tube feeding complications arise, early recognition can prevent serious health consequences and improve patient outcomes.
You’ll need to monitor patients systematically for critical warning signs that indicate potential problems.
Watch for aspiration indicators including sudden coughing, choking sounds, wet vocal quality, or respiratory distress. Recognizing aspiration signs requires immediate assessment of lung sounds and oxygen saturation levels.
For determining feeding tolerance, observe gastric residual volumes, abdominal distention, nausea, vomiting, or diarrhea. High residual volumes above established thresholds suggest delayed gastric emptying. Document feeding interruptions and patterns carefully.
Additional red flags include tube displacement, blockages, or skin irritation around insertion sites.
You’ll also want to monitor electrolyte imbalances and nutritional markers. Quick identification enables prompt interventions, protecting vulnerable patients from preventable complications.
Resolving Clogged and Blocked Feeding Tubes
Because clogged feeding tubes represent one of the most frequent complications in enteral nutrition, you’ll need systematic approaches to restore patency quickly and safely.
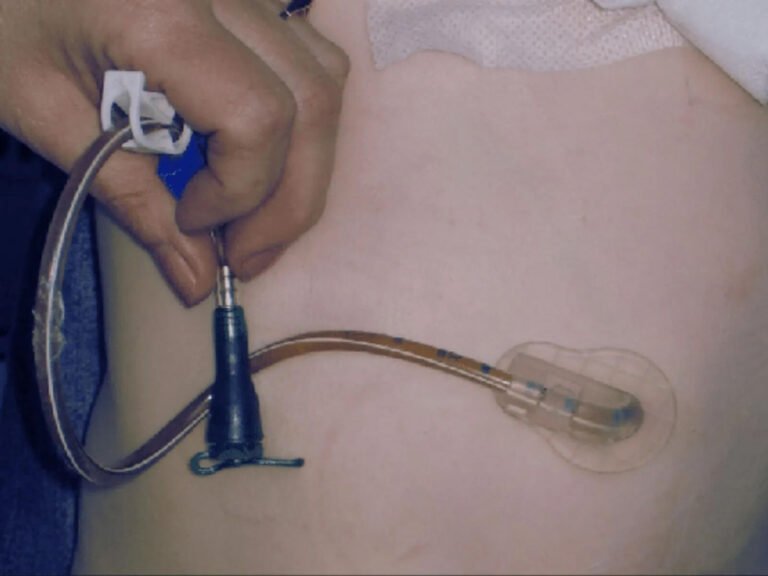
Start with gentle warm water flushes using a 60mL syringe, applying steady pressure rather than forceful pushing that could rupture the tube. If water doesn’t work, try pancreatic enzyme solutions or commercial declogging agents designed specifically for feeding tubes.
Apply steady, gentle pressure with warm water flushes using a 60mL syringe to avoid tube rupture and restore patency safely.
For stubborn blockages, alternate between warm water and carbonated beverages, allowing each to dwell for 15-20 minutes before attempting gentle aspiration.
Prevention remains your best strategy—establish consistent tube cleaning protocols with water flushes before and after each feeding, crush medications thoroughly, and dilute thick formulas appropriately.
Document all interventions and notify physicians when mechanical methods fail, as tube replacement may become necessary.
Managing Formula Intolerance and Digestive Issues
While mechanical blockages pose significant challenges, formula intolerance and digestive complications affect an even larger percentage of tube-fed patients and require equally systematic assessment approaches.
You’ll need to evaluate symptoms like nausea, vomiting, diarrhea, or abdominal distension methodically. Start by reviewing current formula selection against patient-specific needs.
Consider switching to elemental or semi-elemental formulas for compromised digestion. Reduce infusion rates temporarily, then gradually increase as tolerance improves. You can also implement digestive enzymes when pancreatic insufficiency is suspected.
Monitor gastric residuals closely and assess feeding schedules. Sometimes dividing volumes into smaller, more frequent feeds resolves issues.
Document all interventions and patient responses meticulously. If symptoms persist despite these modifications, consult with registered dietitians and gastroenterologists for specialized formula recommendations.
Addressing Tube Displacement and Positioning Problems
Although tube displacement represents one of the most serious complications in enteral nutrition, you can minimize risks through systematic verification protocols and prompt intervention strategies.
Always verify tube placement before each feeding using multiple methods: aspirate gastric contents, check pH levels, and measure external tube markings. If you suspect displacement, stop feeding immediately and notify the healthcare provider.
Monitor your patient’s comfort levels continuously—signs of distress, coughing, or difficulty breathing may indicate malposition. Secure tubes properly using appropriate tape or holders to prevent migration.
Document external measurements at each shift change to track movement. Never attempt to reposition displaced tubes yourself; this requires medical assessment and potential imaging studies.
Quick recognition and professional intervention protect your patients from aspiration pneumonia and other serious complications.
Fixing Equipment Malfunctions and Pump Errors
When enteral feeding pumps malfunction, your swift troubleshooting skills directly impact patient safety and nutritional outcomes. Begin with systematic equipment inspection, checking power connections, tubing alignment, and display error codes. Regular pump calibration guarantees accurate flow rates and prevents medication errors.
| Error Type | Common Causes | Immediate Actions |
|---|---|---|
| Occlusion Alarm | Kinked tubing, clogged line | Check tube pathway, flush gently |
| Low Battery | Inadequate charging, old battery | Connect to power, replace battery |
| Air Detection | Loose connections, empty bag | Secure fittings, prime tubing |
| Flow Rate Error | Incorrect programming, pump drift | Verify settings, recalibrate |
| Door Open Alert | Improperly seated tubing | Reposition tubing, close door |
Document all interventions and contact biomedical engineering when basic troubleshooting fails. Your vigilance protects patients from nutritional interruptions.
Preventing Future Complications Through Proper Maintenance
Since equipment failures often stem from inadequate maintenance protocols, you’ll greatly reduce complications by implementing systematic preventive care routines.
Establish an extensive maintenance schedule that includes daily equipment inspections, weekly deep cleaning, and monthly component replacements. Document each maintenance activity to track patterns and identify potential issues before they compromise patient safety.
Prioritize tube hygiene through consistent flushing protocols using sterile water or saline solutions. Clean feeding sets every 24 hours and replace them according to manufacturer guidelines. Inspect tubing for cracks, kinks, or blockages during each shift change.
Calibrate pumps monthly and maintain backup equipment readily available. Train all staff members on proper handling techniques and emergency procedures.
Your proactive approach to maintenance directly impacts patient outcomes and reduces costly equipment failures.
Conclusion
You’ve Got This!
You’ve learned important skills to handle tube feeding problems. These skills will help keep you or your loved one safe and healthy. Think of yourself as a guardian—watching over every detail with caring eyes and gentle hands.
Check the feeding tube each day, just like you’d check on someone you love. Keep everything clean. Follow the instructions that came with your equipment. These simple steps can stop small problems before they become big ones.
But remember—you’re never alone in this journey. When something doesn’t feel right or a problem won’t go away, it’s time to call your healthcare team. That’s what they’re there for. There’s no such thing as a silly question when it comes to someone’s health.
Your attention and care make all the difference. By staying alert and acting quickly when issues come up, you’re giving the best possible care. You’re preventing serious problems that could lead to hospital visits.
The bottom line? Trust your instincts. Stay informed. And know that help is always just a phone call away.
If you or a loved one need help, don’t wait. Reach out to Skilled Trach Care today at (561) 677-8909 or email us at info@skilledtrachcare.com.