Your child’s speech and swallowing abilities develop through shared anatomical structures—the oral cavity, pharynx, and larynx—that coordinate both functions simultaneously. From birth through age three, neurological maturation enables the shift from reflexive feeding to voluntary control, while cranial nerves refine orofacial movements for both safe swallowing and clear articulation. Watch for red flags like persistent coughing during feeds, absent babbling by twelve months, or extreme texture aversions. Evidence-based interventions and early support strategies can greatly enhance your child’s developmental outcomes when concerns arise.
Key Takeaways
- Speech and swallowing share anatomical structures including the oral cavity, pharynx, larynx, tongue, and velum for coordinated function.
- Infants progress from reflexive feeding to voluntary control, developing first words and managing solid foods by twelve months.
- Cranial nerves and neural pathways mature through myelination, enabling refined oral-motor coordination for both speech and swallowing.
- Warning signs include persistent coughing during feeds, absent babbling by twelve months, and extreme texture aversions requiring assessment.
- Therapeutic interventions like oral-motor exercises, texture modifications, and parent coaching effectively support delayed speech and swallowing development.
The Interconnected Anatomy of Speech and Swallowing
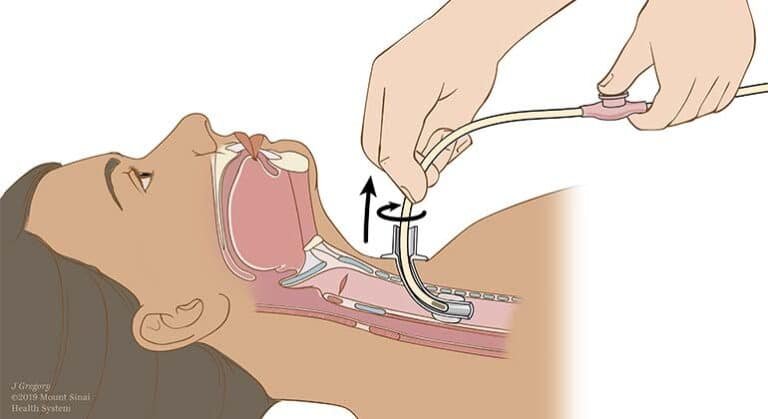
The structures responsible for speech and swallowing share nearly identical anatomical pathways, creating an intricate system where both functions rely on precise coordination of the oral cavity, pharynx, and larynx.
When you’re evaluating patients, you’ll notice how these anatomy connections facilitate both protective and communicative functions. The tongue, velum, and vocal folds serve dual roles—enabling articulation while safeguarding the airway during deglutition.
Understanding these speech pathways helps you identify why disorders in one domain often affect the other. The pharyngeal constrictors that propel food boluses also shape resonance for voice production.
Similarly, laryngeal elevation protects against aspiration while modulating pitch and intensity. This shared infrastructure demands your careful consideration when examining developmental delays or acquired deficits, as intervention strategies must address both functional systems simultaneously.
Developmental Milestones From Birth Through Early Childhood
Newborns enter the world with reflexive feeding patterns that’ll evolve into voluntary, coordinated movements for both nutrition and communication over the first three years of life.
You’ll observe rooting and sucking reflexes shift to purposeful bottle or breast feeding by two months. Around six months, infants develop the oral-motor control necessary for pureed foods while producing early communication sounds like babbling.
By twelve months, they’ll manage soft table foods and speak their first words, demonstrating the parallel maturation of feeding skills and speech.
Between eighteen and thirty-six months, children refine chewing patterns for varied textures while expanding their vocabulary exponentially.
Understanding these developmental sequences helps you identify delays early, enabling timely intervention. Each milestone represents neurological maturation, muscular coordination, and sensory integration working synchronously.
Neurological Maturation and Muscle Coordination
Behind every feeding and speech milestone lies a complex orchestration of neural pathways developing from the brainstem through the cortex.
You’ll observe how myelination of cranial nerves progresses systematically, enabling refined orofacial control essential for both swallowing safety and articulation precision. The trigeminal, facial, glossopharyngeal, vagus, and hypoglossal nerves must achieve synchronized function through repetitive sensorimotor experiences.
As you support developing children, recognize that muscle integration doesn’t occur in isolation.
The coordination between respiratory muscles, laryngeal structures, and oral-pharyngeal musculature requires thousands of practice opportunities. Neuroplasticity allows compensatory pathways when typical development is disrupted, though early intervention optimizes outcomes.
Understanding this neurological foundation helps you identify when developmental trajectories deviate from expected patterns, enabling timely referrals that preserve both nutritional adequacy and communicative potential.
Warning Signs and Red Flags for Developmental Delays
When caregivers report persistent coughing during feeds, frequent respiratory infections, or prolonged mealtimes beyond 30 minutes, you’re hearing critical indicators that warrant immediate assessment.
These warning signs of developmental delays require your clinical attention and timely intervention. Watch for absent babbling by 12 months, limited sound variety, or regression in previously acquired skills.
Oral-motor concerns include tongue thrust beyond 6 months, difficulty shifting textures, or consistent food refusal. You’ll need to document aspiration indicators: wet vocal quality, choking episodes, or recurrent pneumonia.
Delayed self-feeding skills, extreme texture aversions, and failure to meet age-appropriate milestones signal potential dysphagia or speech-language disorders. Your early recognition and referral to specialized services can greatly improve outcomes for these vulnerable children.
Therapeutic Interventions and Early Support Strategies
Once you’ve identified developmental concerns, implementing evidence-based therapeutic interventions becomes your priority to enhance outcomes. Early intervention greatly impacts long-term prognosis, with research demonstrating ideal neuroplasticity during critical developmental windows.
Speech-language pathologists employ targeted therapeutic techniques tailored to each child’s specific needs. For feeding difficulties, you’ll implement oral-motor exercises, sensory integration strategies, and modified texture protocols.
Individualized therapeutic approaches combine oral-motor exercises, sensory strategies, and texture modifications to address each child’s unique feeding challenges effectively.
Articulation disorders respond to phonological awareness activities and motor-speech drills. You’ll collaborate with families to establish home practice routines, ensuring carryover between clinical sessions. Parent coaching empowers caregivers as active participants in their child’s progress.
Augmentative communication devices support children with severe expressive delays. Regular progress monitoring through standardized assessments guides treatment modifications.
Multi-disciplinary coordination with occupational therapists, pediatricians, and educators creates extensive support systems that address underlying developmental challenges holistically.
Conclusion
You’ve learned how speech and swallowing develop through interconnected anatomical structures and neurological pathways. You’re now equipped to recognize typical milestones and identify warning signs that warrant professional evaluation. If you’re concerned about your child’s development, don’t wait—early intervention yields the best outcomes. Contact a speech-language pathologist for thorough assessment. Remember, you’re your child’s best advocate, and evidence-based therapy can greatly improve both communication and feeding skills when challenges arise.