Your child has a tracheostomy, and you’re anxious about sending them to school. Will the teachers understand? Can the nurse handle emergencies? Will your child be treated normally or isolated? With proper planning, trained staff, and the right protocols in place, children with tracheostomies thrive in school, make friends, participate in activities, and experience normal childhood. This comprehensive guide walks you through school coordination, 504 plans, staff training, and peer integration so your child gets the education and social experience they deserve.
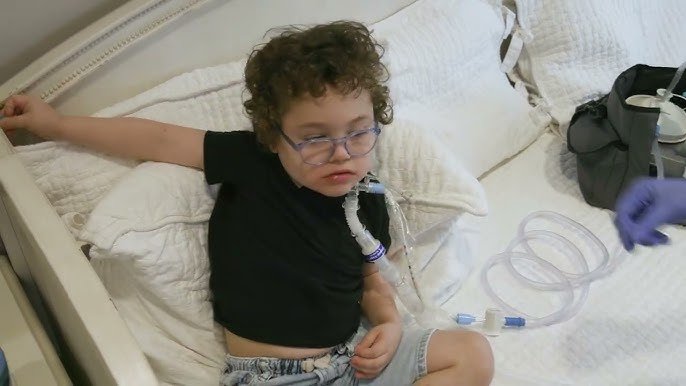
School is where children develop academically, socially, and emotionally. For children with tracheostomies, proper school coordination ensures they access education safely while experiencing normalcy with peers. Research shows that children with complex medical needs who attend regular schools have better outcomes—academically, socially, and developmentally—compared to those excluded or home-schooled.
Before school starts, request meetings with:
Key Message: "My child can attend school safely with trained staff and proper protocols. We'll provide training, equipment, and support."
Prepare a comprehensive packet including:
Initiate formal 504 Plan meeting (federal requirement under Section 504 of the Rehabilitation Act):
What staff should do:
What staff should do:
What staff should do:
School nurse must receive hands-on training in:
We recommend:
Teachers don't need to perform medical care but should understand:
Effective teacher messaging to class:
This normalizing approach prevents stigma and promotes peer acceptance.
Most children with tracheostomies can participate in:
Physician may restrict:
Approach: Maximize inclusion while maintaining safety. Physician determines necessary restrictions.
Age-appropriate explanations help peers normalize the trach:
Clear policies needed:
Each school transition requires coordination:
Additional considerations as child becomes teenager:
Yes, absolutely. With proper planning, trained staff, and emergency protocols in place, trach children attend regular classrooms, participate in activities, and socialize with peers normally. Many schools successfully support trach-dependent children.
A 504 plan is a federal accommodation plan (under Section 504 of Rehabilitation Act) that outlines your child's medical needs and school accommodations including: medical care protocols, emergency procedures, equipment at school, activity modifications, and staff training requirements. Schools are legally required to develop 504 plans for children with medical needs.
The school nurse must receive comprehensive hands-on training in suctioning, tube management, emergency response, and equipment troubleshooting. Teachers should understand basics (when to alert nurse, recognizing problems). All staff working with your child needs awareness training. We can provide specialized training.
Your emergency plan details procedures. Generally: alert school nurse, nurse assesses breathing status, attempt re-insertion if trained (with backup tube), call parent/emergency contact, and call 911 if respiratory distress or unable to reinsert within protocol timeframe. Regular practice drills ensure readiness.
Many trach children safely participate in activities. Most non-contact sports (basketball, soccer, swimming, track) are allowed. Contact sports with neck trauma risk (football, wrestling) typically restricted. Each child's participation determined by physician, condition severity, and school policy. Discuss with your doctor.
Schools are legally required to provide accommodations for students with medical needs under Section 504 and Americans with Disabilities Act (ADA). If school refuses: document all communications, contact your state's disability advocacy organization, and consult with a special education attorney if necessary. Most disputes resolve through proper advocacy.
We provide comprehensive school support including:
Get Expert School Coordination Support
Call: 1 561 677 8909
Available 24/7 | School Coordination Experts | South Florida Service
Learn More About Pediatric Trach Care: